Varicose veins in the lower limbs are common in men and women, especially from adulthood, and this condition can affect quality of life.
Although they are often viewed as an aesthetic problem, varicose veins can cause uncomfortable symptoms and require medical supervision, which is why it’s essential to know the warning signs.
What are varicose veins in the lower limbs?
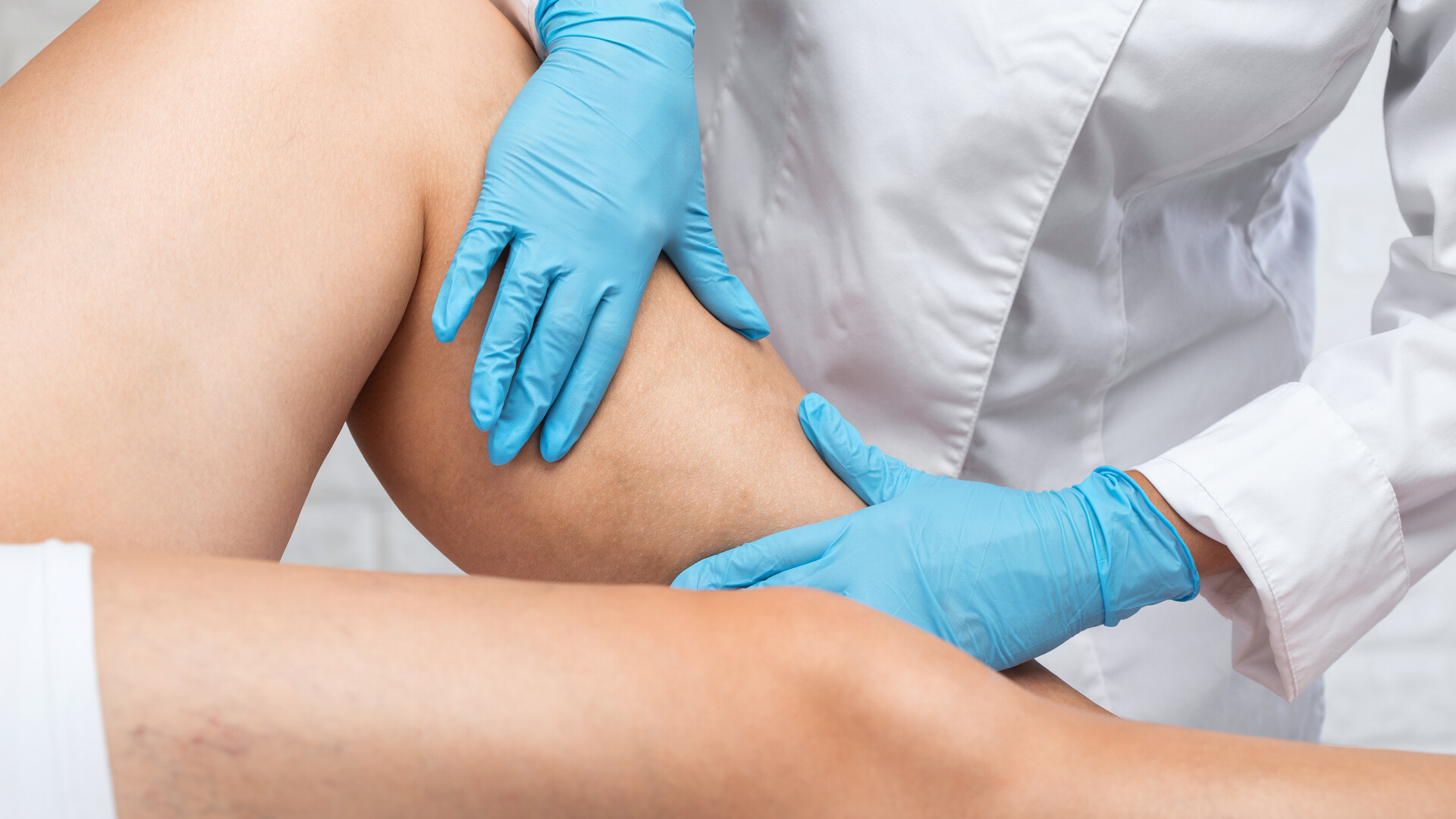
Varicose veins in the lower limbs are dilated and tortuous veins that occur when the venous system fails to function effectively.
Veins in the legs have valves that help blood circulate against gravity, towards the heart. When these valves become impaired, blood tends to pool in the veins, thereby increasing pressure in them and causing them to bulge.
This process is often associated with chronic venous insufficiency (CVI), a condition caused by impaired venous return and which can worsen over time.
What are the symptoms of varicose veins in the lower limbs?
The symptoms can vary from person to person and are not always related to the size or visibility of the varicose veins. We list below some of the most frequent symptoms:
1. Leg fatigue and heaviness
This is one of the most common symptoms, especially at the end of the day or after spending long periods standing or sitting.
2. Pain and discomfort
Pain and discomfort can be localised, or cause a burning sensation or pressure along the affected veins, which can worsen with heat.
3. Swelling (oedema)
It is common for ankles and legs to swell, especially at the end of the day, resulting from impaired venous return (the circulation that returns blood back to the heart).
4. Skin changes
In advanced stages, varicose veins can cause brown blemishes, dry or hardened skin and, in severe cases, venous ulcers.
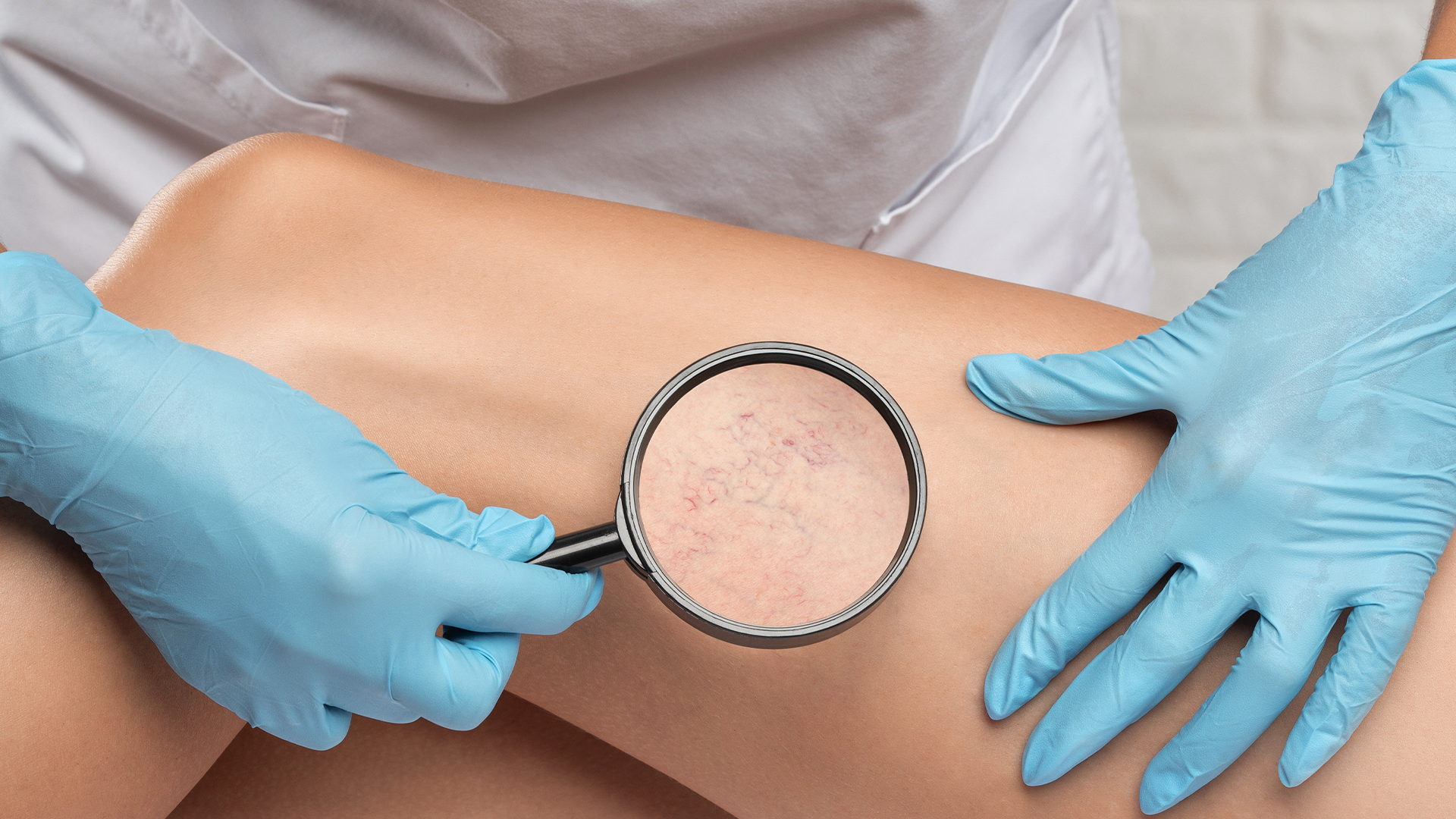
5. Visible and dilated veins
Varicose veins can have a blue or purple appearance, looking swollen and rope-like, visible just under the skin’s surface.