What are the causes of Lipoedema?
The exact cause of lipoedema is still unknown, but we do know that some factors are associated with this condition, namely:
Many women with lipoedema have close relatives (e.g.: mother, grandmother, sisters) with the same problem. This suggests that there is a genetic predisposition, in other words, some families are more likely to develop this condition.
On the other hand, lipoedema usually appears or worsens in phases of major hormonal changes: puberty, pregnancy and menopause. These hormones influence how the body distributes fat. Therefore, in genetically predisposed women, these phases can be “triggers” for the disorder to become apparent.
How is Lipoedema diagnosed?
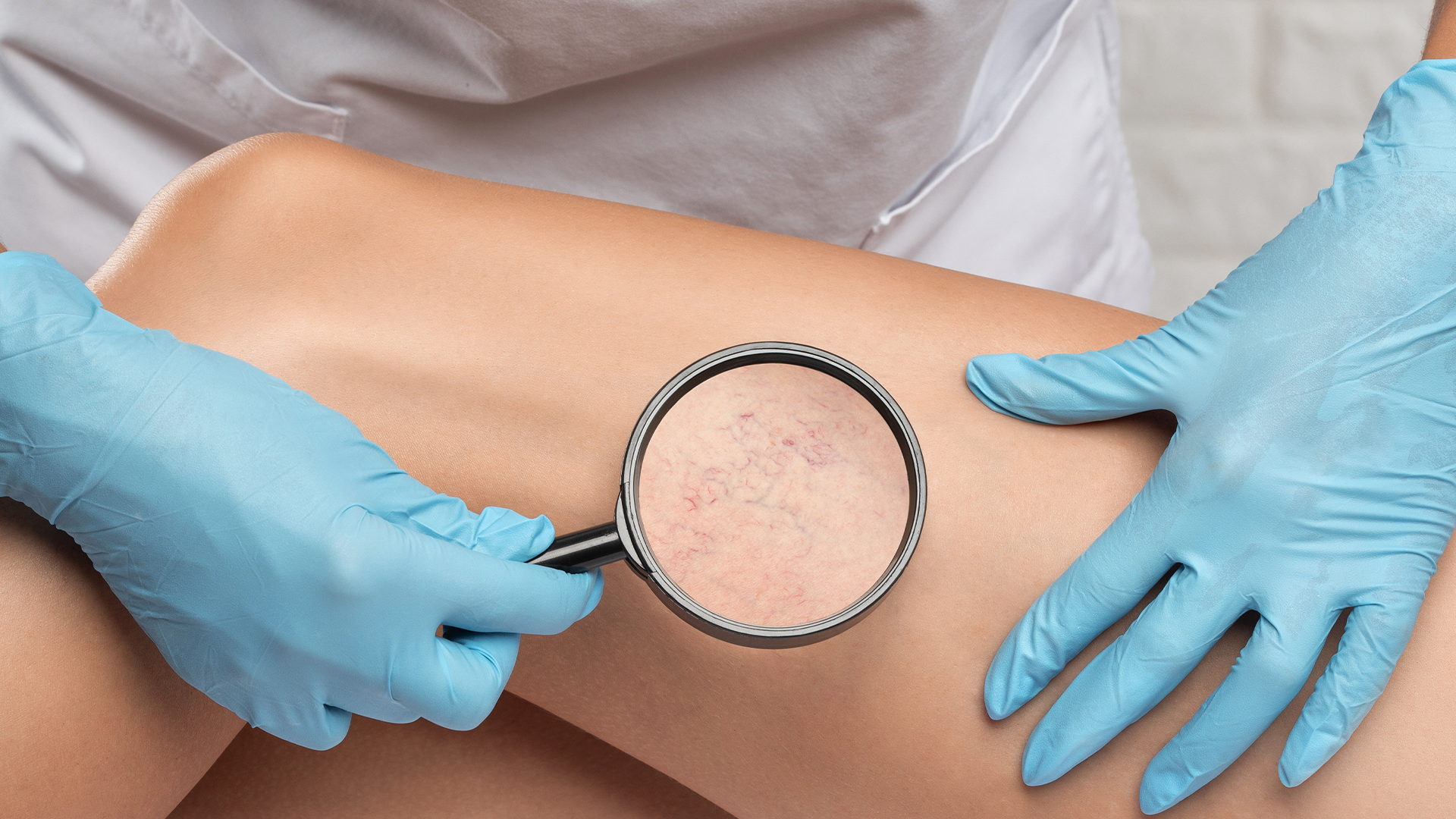
The diagnosis is based on a physical examination and analysis of the symptoms. The physician examines the affected areas and assesses specific signs. The diagnostic approaches include:
- Detailed anamnesis: the physician analyses the patient’s family history (for example, to identify if there is a hereditary component), determining the onset and progression of the condition.
- Physical exam: pressure is applied to assess the sensitivity of the fat deposits; the hands and feet are checked for signs of the disorder; and the physician will also determine if there is a tendency to bruise for no apparent reason.
- Imaging exams: exams such as subcutaneous ultrasound and Doppler ultrasound may be performed to rule out venous disorders; lymphoscintigraphy (maps the lymphatic system) may be prescribed if lymphatic impairment is suspected.
- Ruling out other causes: such as localised adiposity, lipomas, primary lymphoedema or chronic venous insufficiency.
Lipoedema vs lymphoedema: what’s the difference?
Although the names are similar, lipoedema and lymphoedema are different conditions. A person may have just lipoedema, just lymphoedema or both at the same time (a condition called lipo-lymphoedema).
Therefore, an assessment by a specialised professional is extremely important to identify the problem correctly and define the best treatment plan.
Lipoedema
Abnormal fat buildup, especially in the legs, and sometimes the arms. The increase in volume is symmetrical, painful to touch and bruises easily. Hands and feet are usually not affected. Diet and exercise do not substantially reduce this fat.
Lymphoedema
Swelling caused by a disorder in the lymphatic system, which is responsible for draining the body’s fluids. When this system is impaired, the region begins to accumulate fluid, becoming swollen and heavy, possibly hardening over time.
Unlike lipoedema, the swelling can occur on just one side of the body, and it’s common for hands or feet to swell as well.
How is Lipoedema treated?
The treatment for lipoedema is adapted to the patient’s condition and symptoms. Although there is no cure, there are various therapeutic approaches that help control the symptoms and improve quality of life.
These approaches include:
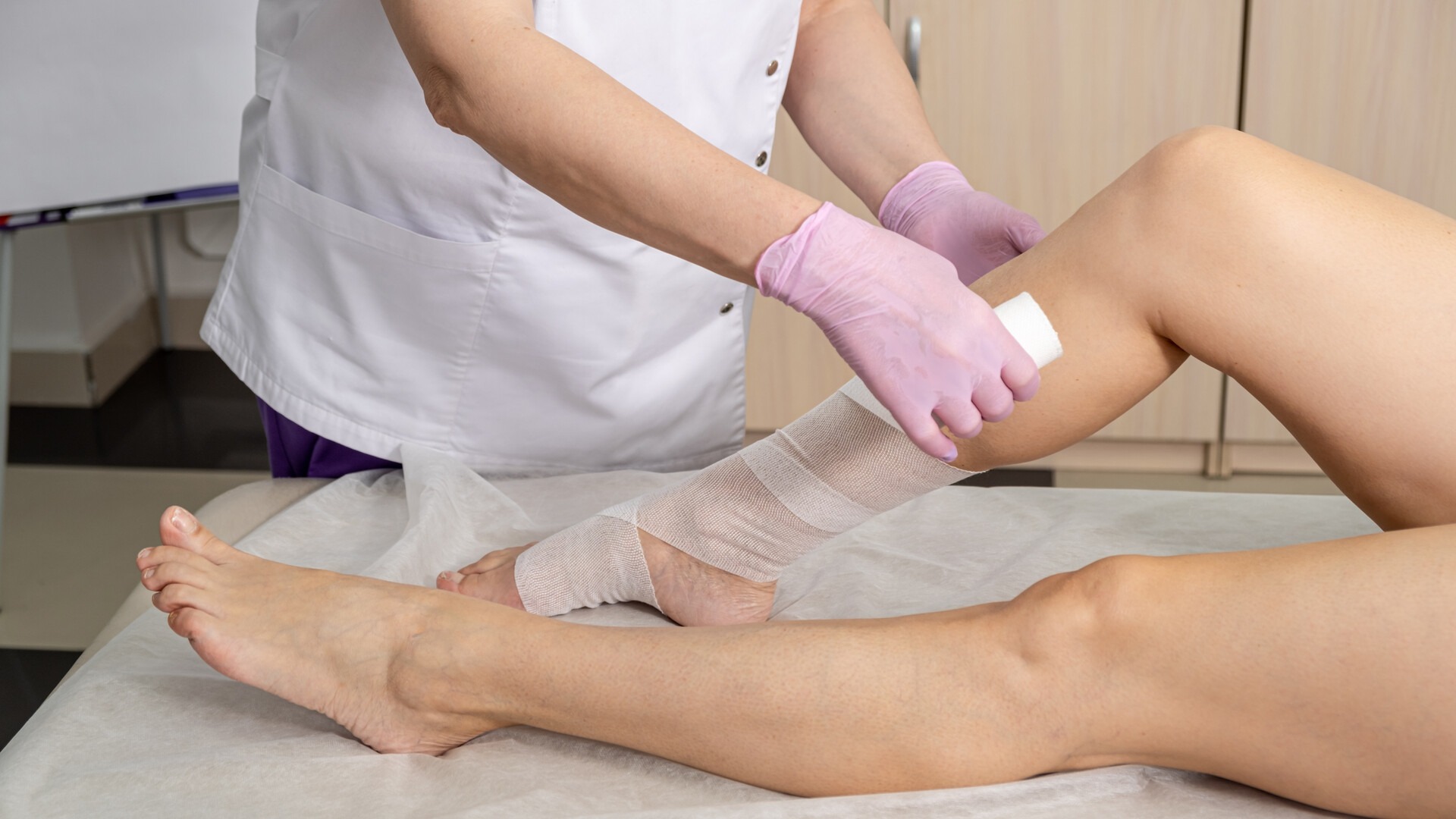
- Compression therapy: applying compression measures that reduce swelling and support the affected areas of the body is advised (these measures are especially important when lymphatic flow is also compromised).
- Manual lymphatic drainage: specialised massage that stimulates the lymphatic system may be recommended to drain excess accumulated fluids.
- Exercise: low intensity activities like walking or swimming help improve blood circulation, thereby reducing swelling.
- Liposuction: this surgical procedure removes accumulated fat, relieving symptoms and improving the patient’s mobility (in specific cases).
- Psychological support and rehabilitation: in some cases, psychological support, physiotherapy for walking, and functional training, as well as nutritional guidance, may be recommended to help improve the person’s everyday life.
Lipoedema: precautions to take?
Although there is no cure for lipoedema, some simple precautions help relieve the patient’s discomfort and improve their daily life:
Avoid remaining in the same position for long periods
Remaining in the same position (standing or sitting) can aggravate the heavy feeling and increase swelling in legs. Therefore, moving the body regularly helps keep circulation active and reduce discomfort at the end of the day.
Wear compression socks
Compression socks help control swelling and the feeling of pressure on legs. These are especially useful on busy days, long trips or in hot weather, when swelling tends to worsen.
Take breaks to activate circulation
Getting up for a few minutes throughout the day, even just to take a few steps, makes a great difference. This simple movement helps the body drain fluids and reduces heaviness in legs.
Maintain a healthy weight
Although lipoedema is not directly associated with weight, being overweight increases the pressure on joints and aggravates discomfort. Maintaining a healthy weight increases mobility and general wellbeing.
Regular, low-impact exercise
Low intensity exercise (e.g.: walking or swimming) helps improve circulation, strengthens muscles and relieves stiffness. For example, water aerobics combine movement with hydrostatic pressure, acting as a natural compressor.
Choose a balanced diet
Choosing fresh and varied foods reduces the body’s inflammatory states and keeps energy levels more stable. Avoiding ultra-processed foods and excessive sugar helps control swelling and increases general wellbeing.
Keep skin well moisturised
Skin affected by lipoedema can become sensitive and dry. Using moisturisers daily strengthens the skin barrier, helps prevent minor wounds or cracks and reduces the risk of rashes.
Maintain regular follow-up
Vigilance and detecting symptoms early are crucial, especially if you have a family history of this condition. Treat any venous/lymphatic component (associated with veins and the lymphatic system) as soon as possible.