Melanoma is the most serious type of skin cancer, with about seven hundred new cases occurring in Portugal every year. Learn what to watch out for and how to treat it.
Melanoma is a type of skin cancer that develops from accumulated mutations in melanocytes (cells responsible for pigmentation) in the skin or mucous membranes. Its incidence has been increasing in both the United States and Europe, including Portugal. Despite its severity, there are currently several innovative treatments for melanoma that provide increasingly better outcomes in its therapeutic approach.
What is melanoma?
Melanoma is a cancer that develops in melanocytes, the cells that produce pigment in the skin. These cells undergo a mutation and multiply at a faster rate than normal cell renewal, accumulating and forming melanoma.
Most of these cells are located in the outermost layer of the skin, called the epidermis, but melanocytes can also be found in other parts of the body, such as the retina of the eyes or mucous membranes. However, most melanomas are cutaneous and can appear on any surface of the skin, especially in areas exposed to the sun. In men, melanoma is more common on the trunk, head, or neck, while in women, it tends to occur on the lower legs.
Melanoma appears as a "mole" on the skin and is considered one of the most dangerous types of cancer due to its ability to metastasize rapidly to other organs. On the other hand, it is a curable cancer. Therefore, it is crucial to be aware of the main warning signs in order to initiate treatment at an early stage and improve the prognosis.
What are the symptoms of melanoma?
Melanoma symptoms can be observed by the patient at home through a monthly self-examination of the skin. The best time to do this is after bathing or showering, carefully examining the skin in a well-lit area using a full-length mirror and a handheld mirror. All areas of the skin should be checked, including the back, scalp, between the buttocks, and the genital area.
During the observation, pay attention to changes in the skin, especially in moles. It is important to be aware of any birthmarks or moles you may have in order to monitor them and identify any changes.
Therefore, check for new moles with suspicious appearances or changes in size, shape, color, or texture of an existing mole. It is also important to pay attention to wounds that are slow to heal.
Most melanomas appear as an altered mole or a new mole. Generally, they are black or blue-black and have an abnormal appearance that can vary significantly. The ABCDE rule is a good way to distinguish a healthy mole from melanoma:
A. Asymmetry: One half of the mole does not match the other.
B. Border irregularity: The edges of the mole are irregular, without a defined pattern, and the pigment may spread into the surrounding skin.
C. Color: The color of the mole is not uniform and may have different shades or tones.
D. Diameter: The mole is larger than 5 millimeters.
E. Evolution: The mole increases in size over time.
In general, melanoma does not cause pain, but it can cause itching, exudation (release of fluid), or bleeding, especially in more advanced tumors.
If you have any doubts while observing your skin, do not hesitate to consult your dermatologist. However, self-examination guidelines are not meant for making a diagnosis and can never replace a medical examination. Therefore, only a dermatologist should decide whether an anomalous mole should be monitored or removed and analyzed.
What causes skin melanoma?
The exact causes of melanoma are not known. However, several risk factors have been identified that can increase the likelihood of developing the disease. The main ones are described below:
- Heredity: There is a greater risk of developing melanoma when there is a family history of this tumor.
- Exposure to ultraviolet radiation (sun or tanning beds): Sunburns with blisters, especially during childhood, increase the risk of melanoma.
- Skin with many moles: When the skin has a high number of atypical moles or birthmarks, there is a greater likelihood of developing melanoma.
- Fair skin: People with lighter skin tones have a higher risk of developing sunburns and, consequently, melanoma.
- Age: Melanomas more commonly occur in elderly individuals.
How is melanoma diagnosed?
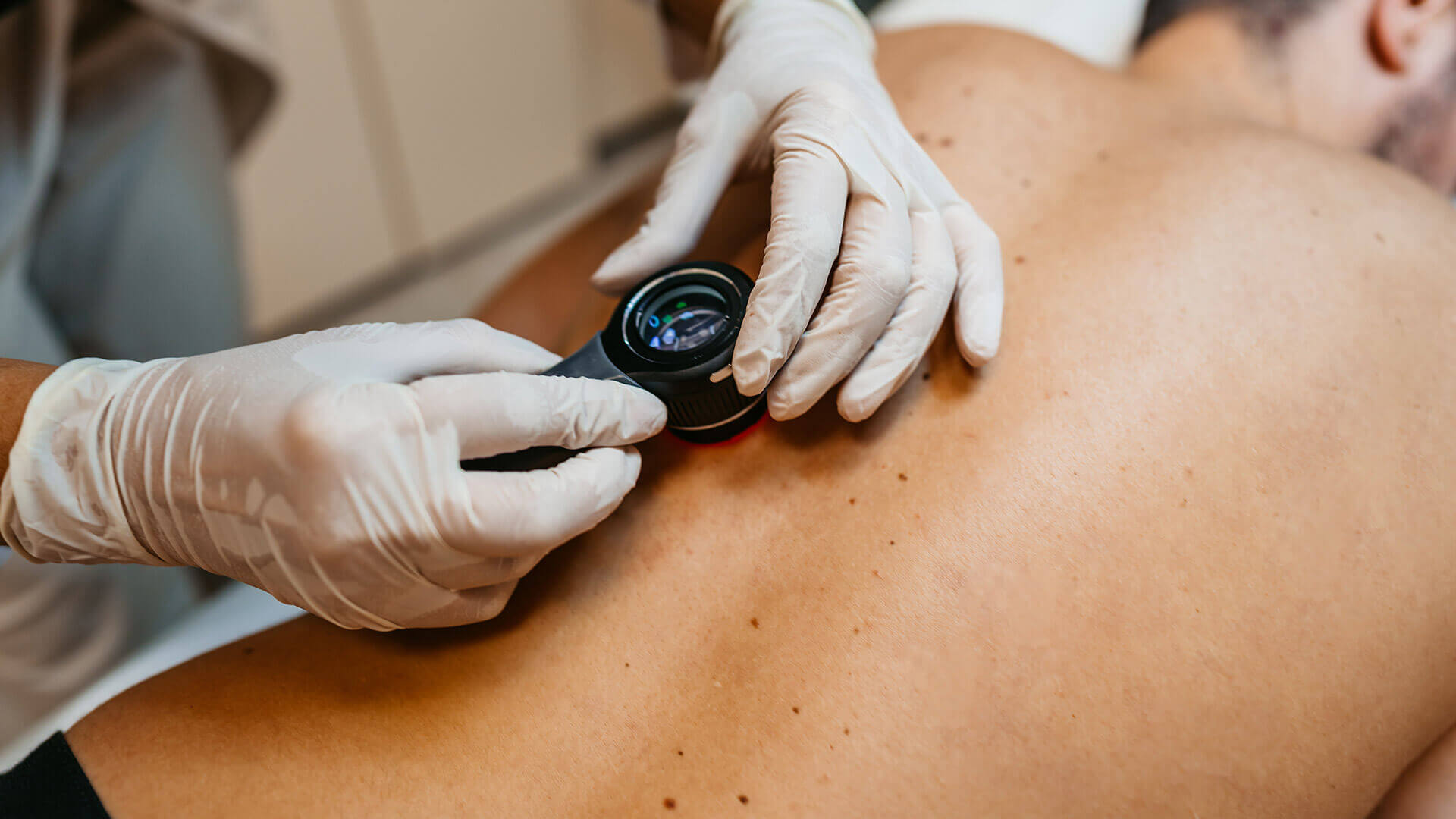
The diagnosis of melanoma is made by a dermatologist who, first and foremost, observes the skin. The doctor will also inquire about sun exposure habits, previous history of moles and skin tumors, and family history of this disease.
In the presence of a suspicious mole, the dermatologist may use a technique called dermatoscopy, which involves shining a special light on the skin to detect subtle changes in moles and identify new high-risk moles.
A biopsy may be necessary to reach a definitive diagnosis. Typically, a biopsy can be performed in the doctor's office under local anesthesia. Tissue is removed to be evaluated in a pathology laboratory and confirm the presence of melanoma cells. If the biopsy reveals the presence of melanoma, the dermatologist will then assess the stage of the disease to determine the most appropriate treatment.
How is the stage of melanoma determined?
The staging of the disease can be determined using various additional tests, as described below:
Sentinel lymph node biopsy:
Sentinel lymph node biopsy is a diagnostic procedure that identifies the first lymph node to receive lymphatic drainage from the tumor. This is typically done using a triple technique. Prior to surgery, a lymphoscintigraphy (an examination to identify lymphatic drainage pathways) is performed by Nuclear Medicine. During surgery, a dye is injected at the site of the lesion, which follows the lymphatic pathway until it reaches the sentinel lymph node. Additionally, a handheld gamma probe is used by the surgeon to locate the sentinel node, previously identified in the lymphoscintigraphy. If melanoma cells are found in this lymph node, it indicates that the melanoma has spread to the lymphatic system. This allows for a more accurate prognosis and the determination of whether adjuvant treatment is necessary.
Imaging tests:
Imaging tests such as computed tomography (CT), magnetic resonance imaging (MRI), or positron emission tomography (PET) provide images of structures within the body, including soft tissues and internal organs. The aim is to confirm whether there is an increase in lymph nodes or lesions in other organs that may be related to the spread of melanoma. Based on these evaluations, the dermatologist, surgeon, and oncologist can assess the tumor's thickness, extent, and invasion of other parts of the body. The staging of melanoma can then be classified according to the TNM system (reference and TNM image).
Melanoma: Treatment
The treatment of melanoma depends on its stage, so it is the responsibility of the multidisciplinary team (including the dermatologist, surgeon, and oncologist who follow the patient) to design the most appropriate therapeutic plan for each case. However, these are the most common treatments:
Surgery
Surgery is the most common and effective treatment for melanoma. It is particularly effective when the primary melanoma is thin and has not spread to the lymph nodes. The tumor and adjacent tissue (referred to as the "margin") are removed to significantly reduce the likelihood of recurrence. In thin melanomas (<0.8mm, without ulceration), margin enlargement is the only procedure required and can sometimes be done under local anesthesia. In advanced stages, excision or margin enlargement, as well as sentinel lymph node biopsy, may be necessary. In cases with extensive lymph node involvement, additional surgery such as lymphadenectomy (removal of all lymph nodes in that area) may be required.
Systemic Treatments
Systemic treatments involve the use of drugs to destroy melanoma cancer cells. They can be administered orally or intravenously, circulating throughout the body. There are several systemic treatments effective in treating melanoma, including immunotherapy and targeted therapies, which can be used for advanced disease or as adjuvant treatment following surgery.
Immunotherapy
Immunotherapy is an intravenous anti-neoplastic treatment that stimulates the immune system, enhancing the body's natural ability to fight cancer. It can be implemented after surgery to minimize the risk of melanoma recurrence.
Targeted Therapies
If melanoma cells have specific mutations in their genes, such as the BRAF gene mutation that occurs in about 50% of melanoma cases, medications in the form of tablets can be used to target and block the altered cellular growth pathway. The combination of BRAF inhibitors and MEK inhibitors can be used in patients with high-risk or metastatic melanomas who have the BRAF gene mutation.
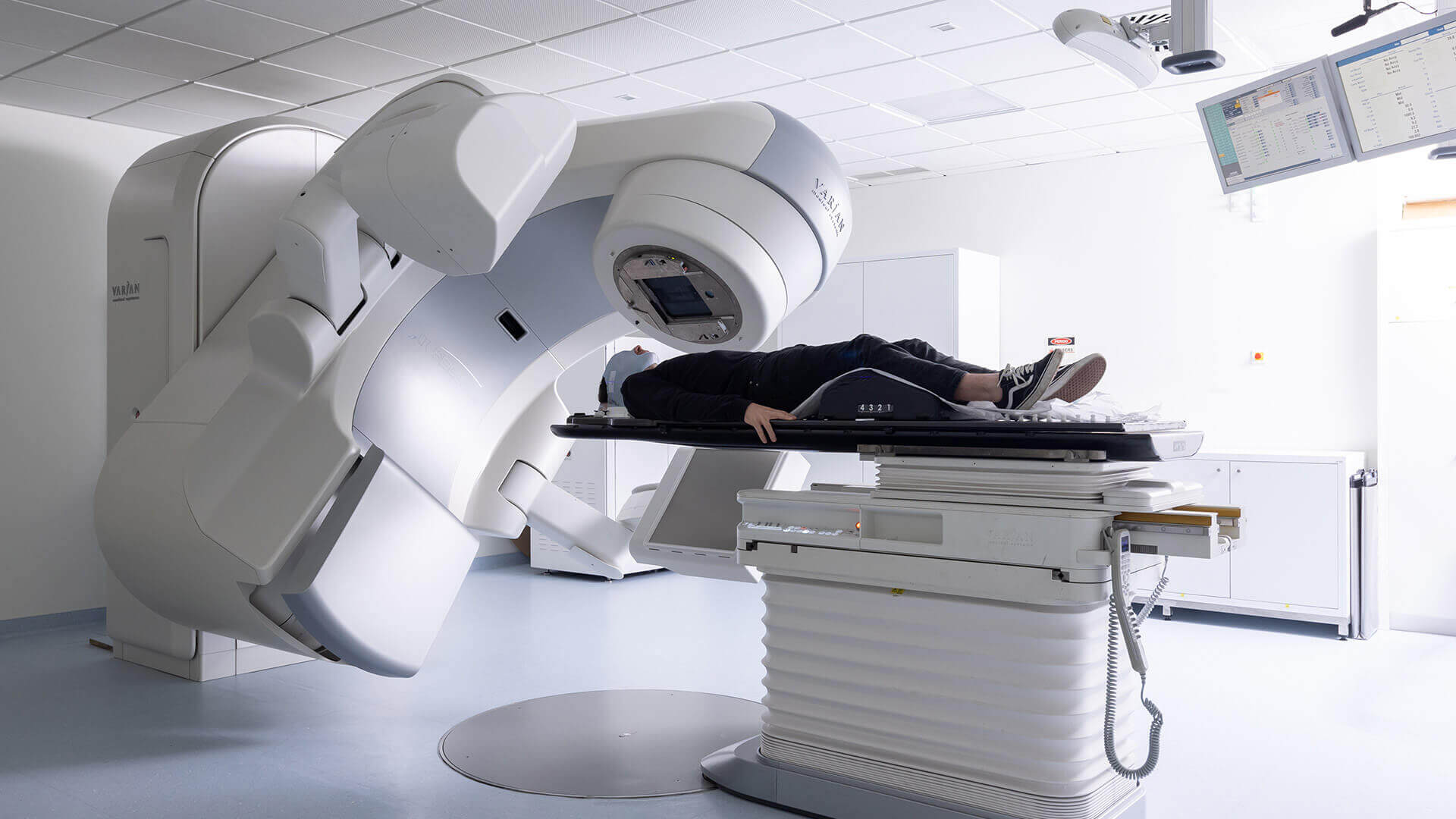
Radiation Therapy
Radiation therapy uses external radiation to destroy cancer cells. It can be used to control the progression of metastasized melanoma, reduce tumor size, or relieve symptoms. This treatment is typically performed on an outpatient basis over several weeks.
Joaquim Chaves Saúde, for the well-being of your skin and melanoma treatment
It is crucial to identify melanoma early. The thickness of the melanoma and lymph node involvement are determining factors for prognosis. If you notice any symptoms or signs with the mentioned characteristics, schedule an appointment with your dermatologist. Do not delay seeking help and take care of your skin now.
At the Skin Oncology Center of Joaquim Chaves Saúde, you will find a multidisciplinary team dedicated to the treatment of melanoma and other skin tumors, with access to the most accurate and advanced diagnostic methods to provide you with the most suitable medical care for your case.